Dyshidrosis: cúiseanna, comharthaí agus cóireálacha
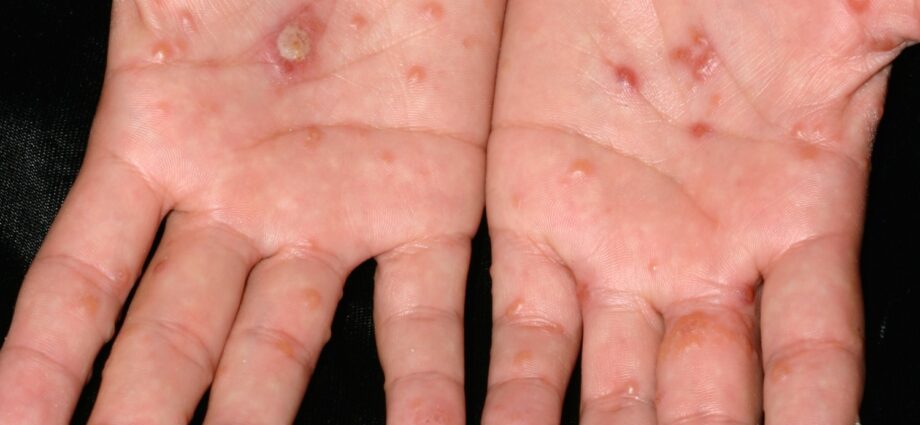
Is coinníoll craiceann é dyshidrosis arb iad is sainairíonna veicilíní ar dhromchlaí cliathánach na méara agus na toes, chomh maith leis na bosa agus na boinn. Bíonn sé go minic, go háirithe sa samhradh.
Sainmhíniú ar dyshidrosis
Is cineál ecsema é dyshidrosis ar a dtugtar dermatosis vesicular na lámha. Ba cheart idirdhealú a dhéanamh idir dyshidrosis ó chineálacha eile ecsema vesiculo-bullous na lámha mar:
- le pompholyx, a fhreagraíonn do gríos tobann pailmeoplantar agus / nó gríos tairbhiúil gan deargadh, agus ina dhiaidh sin déantar díshalannú ar feadh thart ar 2 go 3 seachtaine agus féadfaidh sé tarlú arís
- anecsema vesiculobullous ainsealach ag dul ar aghaidh go minic chuig scoilteadh agus ramhrú an chraiceann
- la dermatosis hyperkeratotic na lámha, De ghnáth bíonn paistí tiubha téada ann a mbíonn tionchar acu ar fhir idir 40 agus 60 bliain d’aois le scoilteanna uaireanta i lár na bosa. De ghnáth bíonn cúiseanna éagsúla leis, ailléirgí teagmhála, greannú agus tráma ainsealach a cheangal (DIY, srl.)
- damáiste mór vesicular tánaisteach do mycóis cosa nó lámha.
Cúiseanna de la dyshidrose
Níl mórán ar eolas faoi na cúiseanna atá le dyshidrosis ach is eol go bhfuil baint aige le coinníollacha eile:
- an ionfhabhtú giosta go dermatophytes mar chos lúthchleasaí
- l 'hipearhidrosis palmoplantar nó sweating méadaithe sna lámha agus na cosa. Mar an gcéanna, is clasaiceach é dysidrosis a fheiceáil le feiceáil sa samhradh nuair a mhéadaíonn an teas.
- anatóp : faighimid stair theaghlaigh nó phearsanta atópachta i roinnt staidéar ach ní i staidéir eile…
- l 'ailléirge miotail (nicil, cróimiam, cóbalt, srl.), plaistigh áirithe (paraphenylene diamine) agus Beaume du Pérou le fáil i roinnt othar
- le tobac d’fhéadfadh sé a bheith ina fhachtóir géaraithe
Diagnóisiú dyshidrosis
Tá dhá chineál dyshidrosis ann:
- dyshidrosis simplí, gan deargadh ag gabháil leis. Níl ach veicilíní ar an gcraiceann
- ecsema dyshidrotic, ag comhcheangal veicilíní agus deargadh nó fiú scálú.
Sa dá chás is minic a bhíonn an itching dian agus féadann sé gríos na blisters a thionlacan nó a thionlacan.
Tá siad seo soiléir (cosúil le “blisters uisce”), go minic siméadrach go garbh ar gach lámh agus cos, is gnách go gcumascann siad, ansin:
- nó triomaíonn siad, ag cruthú crúba donn go minic.
- nó pléascann siad, ag cruthú créacht oozing
Leitheadúlacht dyshidrosis
Tá dyshidrosis ann ar fud an domhain ach is cosúil go bhfuil sé níos annamh san Áise. Tá sé níos coitianta i measc daoine fásta ná i measc leanaí. Baineann sé le fir agus mná araon.
Dealraíonn sé go gcuireann teagmháil athchleachtach le táirgí greannaitheacha (táirgí glantacháin, etc.) agus uisce, chomh maith le caitheamh fada lámhainní, fachtóirí le dyshidrosis. Dá bhrí sin is iad na gairmeacha atá i mbaol géarú dyshidrosis ná báicéirí, búistéirí, cócairí agus ceirdeanna lónadóireachta, ach freisin gairmeacha sláinte agus go ginearálta gach gairm a bhfuil a lámha in uisce nó in atmaisféar te agus tais. .
Éabhlóid agus deacrachtaí féideartha dyshidrosis
Is minic a bhíonn an éabhlóid athfhillteach, uaireanta poncaithe ag na séasúir (atarlú san earrach nó sa samhradh mar shampla). Uaireanta, bíonn veicilíní dyshidrosis ionfhabhtaithe: bíonn a n-ábhar níos gile (purulentach) agus féadann siad lymphangitis, nód lymph san armpit nó groin a chur faoi deara…
Comharthaí an ghalair
Sainmhínítear dyshidrosis de réir chuma blisters itchy ar na lámha agus na cosa. Ceachtar nach bhfuil deargadh ag gabháil leo, is dyshidrosis simplí é.
Nó tá deargadh nó fiú feannadh ann, labhraímid faoi ecsema mhiasidrotic:
- Ar na cosa: is minic a aimsítear an deargadh ar bharraicíní, i log na coise agus ar dhromchlaí cliathánach na gcosa
- Ar na lámha: tá siad níos coitianta ar na méara agus ar aghaidh na palmar
Fachtóirí riosca le haghaidh dyshidrosis
Is iad na fachtóirí riosca le haghaidh dyshidrosis:
- an ionfhabhtú giosta cosa agus lámha le dermatophytes cosúil le cos lúthchleasaí
- l 'hipearhidrosis palmoplantar nó sweating méadaithe sna lámha agus na cosa.
- an ailléirgí miotail (nicil, cróimiam, cóbalt, srl.), plaistigh áirithe (paraphenylene diamine) agus Beaume du Pérou
- le tobac a d’fhéadfadh a bheith ina fhachtóir géaraithe teagmháil athchleachtach le táirgí greannaitheacha (táirgí glantacháin, etc.), uisce nó atmaisféar te agus tais agus caitheamh fada lámhainní
Tuairim ár ndochtúir Is fadhb neamhurchóideacha craiceann í dyshidrosis ach luaitear go minic í i gcomhairliúchán mar gheall ar an itching fíochmhar is cúis leis. Bíonn eagla ar othair go dtarlóidh siad arís agus go minic bíonn feadán uachtar réidh le húsáid… Mar sin féin, ní mór dúinn eagla a bheith orainn roimh úsáid ainsealach corticosteroidí tráthúla, foinsí deacrachtaí fadtéarmacha (go háirithe atrophy craiceann) agus spleáchas. Mar sin ní mór don dochtúir a iarraidh ar a chuid othar na tosca a chuireann leis a theorannú agus gan corticosteroidí tráthúla a úsáid ach amháin i gcás géarchéime, ar feadh cúpla lá amháin agus ansin iad a stopadh. Dr Ludovic Rousseau |
Cosc ar dyshidrosis
Tá sé deacair dyshidrosis a chosc toisc go dtarlaíonn athiompaithe uaireanta fiú agus meas ar fhachtóirí rannpháirteacha a sheachaint:
- teorannú perspiration,
- Teagmháil le glantaigh (táirgí tí…),
- teagmháil fhada leuisce agus níocháin láimhe go minic…
I measc na mbeart atá le glacadh chun an riosca athiompaithe a theorannú tá:
- Seachain teagmháil le irritants agus uisce.
- Seachain teagmháil le táirgí a bhfuil tú ailléirgeach leo má tá ailléirge teagmhála aitheanta ag an dochtúir
- Stop caitheamh tobac a d’fhéadfadh a bheith ina fhachtóir a chuireann leis.
- Troid i gcoinne perspiration i gcáshipearhidrosis
Cóireálacha le haghaidh dyshidrosis
Tá an chóireáil áitiúil bunaithe ar corticosteroidí tráthúla cumhachtacha (toisc go bhfuil craiceann na lámha agus na gcosa tiubh), mar Diabhaltach, is minice a chuirtear i bhfeidhm in uachtair, tráthnóna le laghdú de réir a chéile ar líon na n-iarratas
Is féidir le teiripe UV (UVA nó UVB), a chuirtear i bhfeidhm go barrmhaith ar na lámha agus na cosa i dtimpeallacht leighis, dysidrosis agus líon na mbladhmanna a laghdú
Heliotherapy, cur chuige comhlántach i leith dyshidrosis
Is éard atá i heititeiripe ná na lámha agus na cosa a mbíonn tionchar acu orthu a nochtadh go measartha (5 nóiméad sa lá) don ghrian atá ag dul in olcas, timpeall 17 in sa samhradh. Tá sé cosúil ó thaobh meicníochta le teiripe UV a sheachadtar chuig oifig an dochtúra.