Clár ábhair
Cóireálacha míochaine don eitinn
Diagnóiseacha
Le linn chéim ghníomhach an ghalair, bíonn comharthaí i láthair de ghnáth (fiabhras, allas oíche, casacht leanúnach, srl.). Braitheann an dochtúir ar na hairíonna seo, ach freisin ar thorthaí na dtástálacha agus na scrúduithe seo a leanas.
Tástáil craicinn. Is féidir leis an tástáil chraiceann láithreacht bacillus Koch a bhrath sa chorp. I duine nua-ionfhabhtaithe, beidh an tástáil seo dearfach 4 go 10 seachtaine tar éis an ionfhabhtaithe. Méid beag bídeach eitinn (próitéin íonaithe ó Mycobacterium eitinn) a instealladh faoin gcraiceann. Má tharlaíonn imoibriú craiceann ag suíomh an insteallta (deargadh nó at) sna 48 go 72 uair an chloig eile, léiríonn sé seo ionfhabhtú. Má tá an toradh diúltach, féadfaidh an dochtúir an dara tástáil a mholadh cúpla seachtain ina dhiaidh sin.
Cóireálacha míochaine don eitinn: tuig gach rud i 2 nóiméad
Radagrafaíocht scamhógach. Má tá comharthaí casachta leanúnach ag an othar, mar shampla, ordófar x-gha cófra chun riocht na scamhóga a mheas. Le linn na gníomhaíochta leantacha, is féidir leis an x-gha dul chun cinn an ghalair a sheiceáil.
Tástálacha bitheolaíocha ar shamplaí secretion scamhógach. Breathnaítear na rúin ar dtús faoi mhicreascóp chun a sheiceáil an bhfuil na baictéir atá sna rúin mar chuid den teaghlach mycobacteria (is mycobacterium é bacillus Koch). Faightear toradh na tástála seo an lá céanna. Leanaimid ar aghaidh chuig an cultúr rúin baictéir a aithint agus cibé an bhfuil siad frithsheasmhach in aghaidh antaibheathach nó nach bhfuil. Mar sin féin, caithfidh tú fanacht 2 mhí chun na torthaí a fháil.
Má nochtann an tástáil mhicreascópach láithreacht mycobacteria agus má thugann an mheastóireacht leighis le tuiscint gur eitinn í, cuirtear tús le cóireáil le antaibheathaigh gan fanacht le toradh na tástála ar chultúr miocróbach. Dá bhrí sin, déantar na hairíonna a mhaolú, déantar an galar a rialú, agus is lú an seans go dtarchuirfidh an duine an t-ionfhabhtú chuig na daoine timpeall orthu. Is féidir an chóireáil a cheartú ansin, más gá.
Cóireálacha antaibheathach
An antaibheathaigh céadlíne in ann an eitinn a bhualadh i mbeagnach gach cás. Iarrtar ar dhaoine a bhfuil an riocht orthu fanacht sa bhaile nó masc a chaitheamh go poiblí go dtí go gcinneann an dochtúir nach bhfuil siad tógálach a thuilleadh (tar éis dhá nó trí seachtaine de chóireáil de ghnáth).
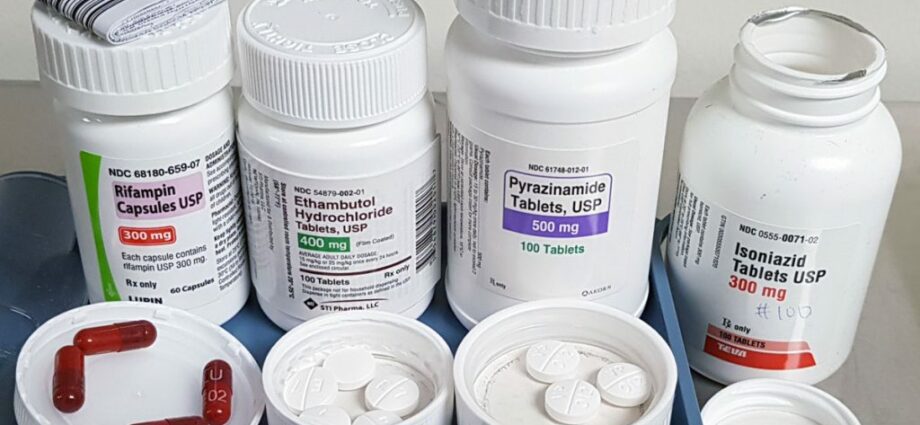
Cóireáil chéad líne. Forordaithe de ghnáth ceithre antaibheathach is iad seo a leanas isoniazid, rifampin, ethambutol agus pyrazinamide, a thógtar trí bhéal. Le bheith éifeachtach agus baictéir a mharú go hiomlán, éilíonn cóireáil leighis go dtógfaí na drugaí go laethúil ar feadh íostréimhse ama. Mhí 6, uaireanta suas le 12 mhí. Is féidir leis na antaibheathaigh seo go léir damáiste ae a dhéanamh go céimeanna éagsúla. Inis do dhochtúir má tharlaíonn aon comharthaí, mar shampla nausea agus vomiting, cailliúint goile, buíochán (radharc buí), fual dorcha, nó fiabhras gan aon chúis le feiceáil.
Cóireálacha dara líne. Má tá na baictéir frithsheasmhach in aghaidh an dá phríomh antaibheathach (isoniazid agus rifampin), tugtar friotaíocht ildrugaí (MDR-TB) air agus is gá dul i muinín drugaí 2e líne. Uaireanta cuirtear 4 go 6 antaibheathach le chéile. Is minic go gcaithfear iad a thógáil thar thréimhse níos faide, uaireanta suas le 2 bhliain. Is féidir leo fo-iarsmaí a chur faoi deara freisin, mar shampla, numbness sna lámha nó na cosa, agus tocsaineacht ae. Déantar cuid acu a riaradh go hinmheánach.
Cóireálacha le haghaidh baictéir ultra-resistant. Má tá brú an ionfhabhtaithe frithsheasmhach in aghaidh roinnt cóireálacha a chuirtear ar fáil de ghnáth ar an gcéad nó an dara líne, úsáidtear cóireáil níos déine agus níos tocsainí, a thugtar go hinmheánach go minic, chun troid i gcoinne an eitinn seo, mar a thugtar air, atá frithsheasmhach go fairsing nó XDR-TB.
Cons-tásca. AN 'alcól agusacetaminophen Tá contraindicated (Tylenol®) le linn na cóireála. Cuireann na substaintí seo níos mó brú ar an ae agus is féidir leo fadhbanna a chruthú.
Eile
I gcás'bia easnamhach, d’fhéadfadh forlíonadh multivitamin agus mianraí a ghlacadh cuidiú leis an ionfhabhtú a chosc ó theacht ar ais4. Ba cheart go bhfabhar glacadh le nósanna itheacháin níos cothroime d’fhonn dlús a chur leis an téarnamh, nuair is féidir. Le haghaidh tuilleadh sonraí faoi na buneilimintí a bhaineann le bia sláintiúil, féach ar ár gcuid Eat Better.
Tábhachtach. Fiú mura bhfuil an galar tógálach a thuilleadh tar éis 2 nó 3 sheachtain de chóireáil, ba cheart leanúint leis an ré fhorordaithe ar fad. Tá cóireáil neamhiomlán nó míchuí níos measa ná gan aon chóireáil. Go deimhin, is féidir le baictéir atá frithsheasmhach in aghaidh antaibheathach a bheith mar thoradh ar chóireáil a gcuirtear isteach uirthi roimh an téarma. Ansin bíonn sé i bhfad níos deacra agus níos mó ama an galar a chóireáil, agus bíonn na cóireálacha níos tocsainí don chorp. Ina theannta sin, is cúis mhór bháis é, go háirithe i measc daoine atá ionfhabhtaithe le VEID. Faoi dheireadh, má dhéantar na baictéir frithsheasmhach a tharchur chuig daoine eile, tá an chóireáil choisctheach neamhéifeachtach ansin. |