Clár ábhair
Glóbailinéim hypogammaic
Laghdú ar leibhéal na gáma-globulins nó inmunoglobulins is ea hypogammaglobulonemia, substaintí a bhfuil ról tábhachtach acu sa chóras imdhíonachta. Is féidir an aimhrialtacht bhitheolaíoch seo a bheith mar gheall ar dhrugaí áirithe a thógáil nó ar phaiteolaíochtaí éagsúla, agus teastaíonn diagnóis thapa ar chuid acu.
Sainmhíniú ar hypogammaglobulonemia
Sainmhínítear hipogammaglobulinemia ag leibhéal gáma-globulin níos lú ná 6 g / l ar leictreafóiréis próitéin plasma (EPP).
Is substaintí a dhéanann cealla fola iad globulins gáma, ar a dtugtar inmunoglobulins freisin. Tá ról an-tábhachtach acu i gcosaintí an choirp. Laghdaíonn hipogammaglobumonemia laghdú níos mó nó níos lú ar chosaintí imdhíonachta. Tá sé annamh.
Cén fáth tástáil gáma globulin?
Is é an scrúdú a cheadaíonn gáma-globulins a chinneadh, i measc rudaí eile, leictreafóiréis próitéiní serum nó próitéiní plasma. Déantar é i gcás amhrais ar ghalair áirithe nó tar éis torthaí neamhghnácha a leanúint le linn na gcéad scrúduithe.
Forordaítear an scrúdú seo i gcás amhrais ar easnamh imdhíonachta humoral i láthair ionfhabhtuithe arís agus arís eile, go háirithe an ENT agus an sféar bronchopulmonary nó meath ar an riocht ginearálta, i gcás amhras faoi il-myeloma (comharthaí: pian cnámh, anemia, ionfhabhtuithe go minic…).
Is féidir an tástáil seo a úsáid freisin tar éis torthaí neamhghnácha a léiríonn méadú nó laghdú ar phróitéin serum, próitéin ard fuail, cailciam fola ard, mínormáltacht i líon na gcealla fola dearga nó na gcealla fola bána.
Conas a dhéantar measúnacht gáma-globulin?
Is é leictreafóiréis próitéiní serum an scrúdú a fhágann gur féidir na globulins gáma a thomhas.
Ligeann an ghnáththástáil bitheolaíochta seo (sampla fola, ón uillinn de ghnáth) cur chuige cainníochtúil chomhpháirteanna próitéine éagsúla an serum (globulins albaimin, alfa1 agus alfa2, globulins beta1 agus beta2, globulin gáma).
Scrúdú simplí is ea leictreafóiréis próitéiní serum a fhágann gur féidir monatóireacht a dhéanamh ar phaiteolaíochtaí iomadúla agus páirt a ghlacadh iontu: siondróim athlastacha, ailsí áirithe, neamhoird fiseolaíocha nó cothaitheacha.
Treoraíonn sé i dtreo na scrúduithe breise is gá (imdhíonadh agus / nó measúnuithe sonracha ar phróitéiní, measúnú haemaiteolaíoch, iniúchadh duánach nó díleá).
Cad iad na torthaí ar féidir a bheith ag súil leo ó mheasúnacht gáma-globulin?
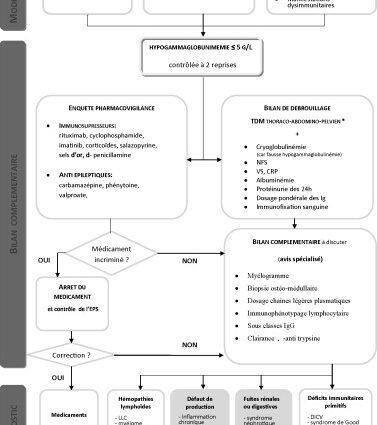
D’fhéadfadh fionnachtain hypogammaglobulonemia a bheith mar thoradh ar dhrugaí a thógáil (teiripe corticosteroid ó bhéal, inmunosuppressants, frith-titimeas, ceimiteiripe meall, srl.) Nó mar gheall ar phaiteolaíochtaí éagsúla.
Ligeann scrúduithe breise diagnóis a dhéanamh nuair a chuirtear cúis an druga as an áireamh.
Chun paiteolaíochtaí ar éigeandálaí diagnóiseacha iad a bhrath (myeloma slabhra éadrom, lymphoma, leoicéime myeloid ainsealach), déantar trí scrúdú: cuardach ar shiondróm meall (lymphadenopathy, hepato-splenomegaly), próitéinuria a bhrath agus comhaireamh fola.
Chomh luath agus a chuirtear na héigeandálaí diagnóiseacha seo as an áireamh luaitear cúiseanna eile hypogammaglobulonemia: siondróm nephrotic, enteropathies exudative. Is féidir le cúiseanna enteropathies exudative a bheith ina ghalar athlastach ainsealach bputóg, galar céiliach chomh maith le siadaí díleácha soladacha nó hemopathies lymphoid áirithe mar lymphoma nó amyloidosis bunscoile (LA, amyloidosis slabhra éadrom inmunoglobulins).
Níos annamh, d’fhéadfadh easnamh imdhíonachta humoral a bheith mar chúis le hypogammaglobulonemia.
Is féidir le míchothú tromchúiseach nó siondróm Cushing a bheith ina chúis le hipogammaglobulonemia freisin.
Ligeann scrúduithe breise an diagnóis a dhéanamh (scanóir thoraco-bhoilg-pelvic, comhaireamh fola, obair athlastach, albuminemia, proteinuria 24 uair an chloig, meáchan a chinneadh inmunoglobulins agus inmunofixation fola)
Conas hypogammaglobulonemia a chóireáil?
Braitheann an cóireáil ar an gcúis.
Is féidir cóireáil choisctheach a chur ar bun i ndaoine atá ag fulaingt ó hypogammaglobulinemia: vacsaíniú frith-niúmacocúil agus vacsaínithe eile, próifiolacsas antaibheathach, ionadú in imdhíonoglobulins ilfhiúsacha.